Power Transformation on Powertransform(Cbind(Chol,hdl,ratio,glyhb,height)~1, Family="Yjpower",diab)
| Hypercholesterolemia | |
|---|---|
| Other names | Hypercholesterolaemia, loftier cholesterol |
 | |
| A color photograph of ii bags of thawed fresh frozen plasma: The bag on the left was obtained from a donor with hypercholesterolemia, and contains altered serum lipid levels, while the handbag obtained from a normal donor contains regular serum lipid levels. | |
| Specialty | Cardiology |
| Complications | Atherosclerosis, thrombosis, embolism, heart assail, stroke, coronary thrombosis, fat embolism, cardiovascular and coronary heart affliction |
| Causes | Poor diet, junk food, fast food, diabetes, alcoholism, monoclonal gammopathy, dialysis therapy, nephrotic syndrome, hypothyroidism, Cushing'southward syndrome, anorexia nervosa |
| Differential diagnosis | Hyperlipidemia, hypertriglyceridemia |
Hypercholesterolemia, also called high cholesterol, is the presence of high levels of cholesterol in the blood.[ane] It is a form of hyperlipidemia (loftier levels of lipids in the blood), hyperlipoproteinemia (high levels of lipoproteins in the blood), and dyslipidemia (any abnormalities of lipid and lipoprotein levels in the claret).[i]
Elevated levels of non-HDL cholesterol and LDL in the blood may be a outcome of nutrition, obesity, inherited (genetic) diseases (such as LDL receptor mutations in familial hypercholesterolemia), or the presence of other diseases such as type 2 diabetes and an underactive thyroid.[1]
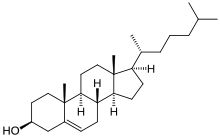
Cholesterol is one of three major classes of lipids which all animal cells employ to construct their membranes and is thus manufactured by all animal cells. Establish cells do manufacture phytosterols (like to cholesterol), just in rather minor quantities.[2] It is also the precursor of the steroid hormones and bile acids. Since cholesterol is insoluble in h2o, it is transported in the blood plasma within protein particles (lipoproteins). Lipoproteins are classified by their density: very low density lipoprotein (VLDL), intermediate density lipoprotein (IDL), depression density lipoprotein (LDL) and high density lipoprotein (HDL).[3] All the lipoproteins carry cholesterol, merely elevated levels of the lipoproteins other than HDL (termed not-HDL cholesterol), particularly LDL-cholesterol, are associated with an increased risk of atherosclerosis and coronary middle disease.[four] In contrast, college levels of HDL cholesterol are protective.[5]
Avoiding trans fats and replacing saturated fats in adult diets with polyunsaturated fats are recommended dietary measures to reduce full blood cholesterol and LDL in adults.[6] [7] In people with very high cholesterol (e.1000., familial hypercholesterolemia), nutrition is often not sufficient to achieve the desired lowering of LDL, and lipid-lowering medications are usually required.[8] If necessary, other treatments such as LDL apheresis or even surgery (for particularly severe subtypes of familial hypercholesterolemia) are performed.[8] About 34 1000000 adults in the United States accept high blood cholesterol.[9]
Signs and symptoms [edit]
Although hypercholesterolemia itself is asymptomatic, longstanding summit of serum cholesterol tin lead to atherosclerosis (hardening of arteries).[10] Over a period of decades, elevated serum cholesterol contributes to formation of atheromatous plaques in the arteries. This can lead to progressive narrowing of the involved arteries. Alternatively smaller plaques may rupture and cause a jell to class and obstruct claret menstruum.[11] A sudden blockage of a coronary artery may upshot in a heart assault. A blockage of an avenue supplying the encephalon tin crusade a stroke. If the development of the stenosis or occlusion is gradual, blood supply to the tissues and organs slowly diminishes until organ function becomes impaired. At this point tissue ischemia (restriction in blood supply) may manifest equally specific symptoms. For case, temporary ischemia of the brain (commonly referred to equally a transient ischemic assault) may manifest as temporary loss of vision, dizziness and impairment of balance, difficulty speaking, weakness or numbness or tingling, ordinarily on one side of the torso. Insufficient blood supply to the heart may cause chest hurting, and ischemia of the eye may manifest every bit transient visual loss in one centre. Insufficient blood supply to the legs may manifest as calf pain when walking, while in the intestines it may present as abdominal pain after eating a repast.[1] [12]
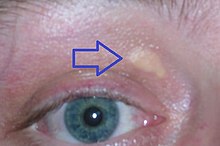
Some types of hypercholesterolemia lead to specific physical findings. For instance, familial hypercholesterolemia (Blazon IIa hyperlipoproteinemia) may be associated with xanthelasma palpebrarum (yellow patches underneath the skin around the eyelids),[13] arcus senilis (white or gray discoloration of the peripheral cornea),[14] and xanthomata (deposition of xanthous cholesterol-rich fabric) of the tendons, peculiarly of the fingers.[15] [sixteen] Type 3 hyperlipidemia may exist associated with xanthomata of the palms, knees and elbows.[xv]
Causes [edit]
Hypercholesterolemia is typically due to a combination of environmental and genetic factors.[10] Environmental factors include weight, diet, and stress.[10] [17] Loneliness is also a risk cistron.[xviii]
Nutrition [edit]
Diet has an effect on blood cholesterol, but the size of this effect varies betwixt individuals.[19] [xx]
A diet high in sugar or saturated fats increases total cholesterol and LDL.[21] Trans fats accept been shown to reduce levels of HDL while increasing levels of LDL.[22]
A 2016 review found tentative evidence that dietary cholesterol is associated with higher claret cholesterol.[23] As of 2018 there appears to be a modest positive, dose-related relationship between cholesterol intake and LDL cholesterol.[24]
Medical conditions and treatments [edit]
A number of other conditions can also increase cholesterol levels including diabetes mellitus type 2, obesity, alcohol utilise, monoclonal gammopathy, dialysis therapy, nephrotic syndrome, hypothyroidism, Cushing's syndrome and anorexia nervosa.[10] Several medications and classes of medications may interfere with lipid metabolism: thiazide diuretics, ciclosporin, glucocorticoids, beta blockers, retinoic acrid, antipsychotics),[10] certain anticonvulsants and medications for HIV too as interferons.[25]
Genetics [edit]
Genetic contributions are usually due to the additive effects of multiple genes ("polygenic"), though occasionally may be due to a unmarried gene defect such as in the case of familial hypercholesterolaemia.[10] In familial hypercholesterolemia, mutations may be present in the APOB gene (autosomal dominant), the autosomal recessive LDLRAP1 gene, autosomal dominant familial hypercholesterolemia (HCHOLA3) variant of the PCSK9 gene, or the LDL receptor gene.[26] Familial hypercholesterolemia affects about one in 250 individuals.[27]
Diagnosis [edit]
| Cholesterol type | mmol/50 | mg/dL | Interpretation |
|---|---|---|---|
| total cholesterol | <5.2 | <200 | Desirable[28] |
| 5.2–vi.2 | 200–239 | Deadline[28] | |
| >6.ii | >240 | High[28] | |
| LDL cholesterol | <ii.6 | <100 | Almost desirable[28] |
| two.half dozen–three.3 | 100–129 | Practiced[28] | |
| 3.4–4.one | 130–159 | Borderline high[28] | |
| iv.1–iv.9 | 160–189 | Loftier and undesirable[28] | |
| >4.9 | >190 | Very loftier[28] | |
| HDL cholesterol | <i.0 | <xl | Undesirable; risk increased[28] |
| one.0–1.5 | 41–59 | Okay, but not optimal[28] | |
| >ane.55 | >60 | Skilful; risk lowered[28] |
Cholesterol is measured in milligrams per deciliter (mg/dL) of blood in the United states of america and another countries. In the Great britain, most European countries and Canada, millimoles per liter of blood (mmol/L) is the measure.[29]
For good for you adults, the UK National Wellness Service recommends upper limits of total cholesterol of 5 mmol/L, and low-density lipoprotein cholesterol (LDL) of iii mmol/50. For people at high risk of cardiovascular disease, the recommended limit for total cholesterol is iv mmol/Fifty, and ii mmol/Fifty for LDL.[30]
In the U.s., the National Heart, Lung, and Blood Institute within the National Institutes of Health classifies total cholesterol of less than 200 mg/dL as "desirable", 200 to 239 mg/dL as "deadline high", and 240 mg/dL or more as "high".[31]
There is no accented cutoff between normal and abnormal cholesterol levels, and values must be considered in relation to other health conditions and risk factors.[ commendation needed ]
College levels of full cholesterol increment the take chances of cardiovascular affliction, particularly coronary heart disease.[32] Levels of LDL or not-HDL cholesterol both predict future coronary center disease; which is the amend predictor is disputed.[33] High levels of small dense LDL may be particularly agin, although measurement of small dense LDL is not advocated for risk prediction.[33] In the past, LDL and VLDL levels were rarely measured directly due to cost. Levels of fasting triglycerides were taken as an indicator of VLDL levels (generally about 45% of fasting triglycerides is equanimous of VLDL), while LDL was usually estimated past the Friedewald formula:
LDL total cholesterol – HDL – (0.2 10 fasting triglycerides).[34]
Even so, this equation is not valid on nonfasting blood samples or if fasting triglycerides are elevated (>four.five mmol/L or >∼400 mg/dL). Recent guidelines have, therefore, advocated the employ of direct methods for measurement of LDL wherever possible.[33] Information technology may be useful to measure all lipoprotein subfractions (VLDL, IDL, LDL, and HDL) when assessing hypercholesterolemia and measurement of apolipoproteins and lipoprotein (a) can likewise be of value.[33] Genetic screening is now advised if a form of familial hypercholesterolemia is suspected.[33]
Classification [edit]
Classically, hypercholesterolemia was categorized by lipoprotein electrophoresis and the Fredrickson classification. Newer methods, such as "lipoprotein bracket assay", have offered significant improvements in agreement the connectedness with atherosclerosis progression and clinical consequences. If the hypercholesterolemia is hereditary (familial hypercholesterolemia), more oftentimes a family history of premature, before onset atherosclerosis is found.[35]
Screening method [edit]
The U.S. Preventive Services Task Force in 2008 strongly recommends routine screening for men 35 years and older and women 45 years and older for lipid disorders and the handling of abnormal lipids in people who are at increased risk of coronary heart disease. They also recommend routinely screening men aged twenty to 35 years and women aged 20 to 45 years if they have other risk factors for coronary heart disease.[36] In 2016 they concluded that testing the general population nether the age of 40 without symptoms is of unclear do good.[37] [38]
In Canada, screening is recommended for men 40 and older and women l and older.[39] In those with normal cholesterol levels, screening is recommended one time every 5 years.[twoscore] Once people are on a statin farther testing provides fiddling benefit except maybe to determine compliance with handling.[41]
Treatment [edit]
Treatment recommendations accept been based on four risk levels for centre disease.[42] For each take a chance level, LDL cholesterol levels representing goals and thresholds for treatment and other activity are made.[42] The higher the risk category, the lower the cholesterol thresholds.[42]
| Gamble category | Criteria for risk category | Consider lifestyle modifications | Consider medication | ||||
|---|---|---|---|---|---|---|---|
| No. of gamble factors† | x-yr gamble of myocardial ischemia | mmol/litre | mg/dL | mmol/litre | mg/dL | ||
| High | Prior heart disease | OR | >20% | >2.six[43] | >100 | >two.6 | >100 |
| Moderately high | 2 or more | AND | 10–xx% | >3.iv | >130 | >3.4 | >130 |
| Moderate | 2 or more | AND | <10% | >three.four | >130 | >4.1 | >160 |
| Depression | 0 or 1 | >4.1 | >160 | >4.9 | >190 | ||
| †Risk factors include cigarette smoking, hypertension (BP ≥140/90 mm Hg or on antihypertensive medication), low HDL cholesterol (<40 mg/dL), family history of premature centre disease, and age (men ≥45 years; women ≥55 years). | |||||||
For those at high adventure, a combination of lifestyle modification and statins has been shown to decrease mortality.[10]
Lifestyle [edit]
Lifestyle changes recommended for those with high cholesterol include: smoking cessation, limiting alcohol consumption, increasing physical activity, and maintaining a good for you weight.[19]
Overweight or obese individuals can lower blood cholesterol past losing weight – on boilerplate a kilogram of weight loss can reduce LDL cholesterol by 0.8 mg/dl.[viii]
Diet [edit]
Eating a diet with a high proportion of vegetables, fruit, dietary fibre, and low in fats results in a modest decrease in total cholesterol.[44] [45] [eight]
Eating dietary cholesterol causes a small but pregnant rise in serum cholesterol,[46] [47] the magnitude of which tin can exist predicted using the Keys[48] and Hegsted[49] equations. Dietary limits for cholesterol were proposed in Us, but non in Canada, United Kingdom, and Australia.[46] Consequently, in 2015 the Dietary Guidelines Informational Committee in the Usa removed its recommendation of limiting cholesterol intake.[50]
A 2020 Cochrane review institute replacing saturated fat with polyunsaturated fat resulted in a small decrease in cardiovascular disease past decreasing claret cholesterol.[51] Other reviews accept not found an effect from saturated fats on cardiovascular disease.[52] [seven] Trans fats are recognized as a potential gamble factor for cholesterol-related cardiovascular disease, and avoiding them in an developed diet is recommended.[vii]
The National Lipid Association recommends that people with familial hypercholesterolemia restrict intakes of full fat to 25–35% of energy intake, saturated fat to less than 7% of energy intake, and cholesterol to less than 200 mg per solar day.[8] Changes in total fat intake in depression calorie diets exercise non appear to affect blood cholesterol.[53]
Increasing soluble cobweb consumption has been shown to reduce levels of LDL cholesterol, with each boosted gram of soluble fiber reducing LDL past an average of ii.2 mg/dL (0.057 mmol/50).[54] Increasing consumption of whole grains likewise reduces LDL cholesterol, with whole grain oats being particularly constructive.[55] Inclusion of two g per 24-hour interval of phytosterols and phytostanols and 10 to xx thou per day of soluble fiber decreases dietary cholesterol absorption.[8] A diet loftier in fructose can raise LDL cholesterol levels in the blood.[56]
Medication [edit]
Statins are the typically used medications, in addition to good for you lifestyle interventions.[57] Statins can reduce total cholesterol past virtually l% in the majority of people,[33] and are effective in reducing the risk of cardiovascular affliction in both people with[58] and without pre-existing cardiovascular disease.[59] [60] [61] [62] In people without cardiovascular illness, statins have been shown to reduce all-crusade mortality, fatal and non-fatal coronary center disease, and strokes.[63] Greater benefit is observed with the use of high-intensity statin therapy.[64] Statins may better quality of life when used in people without existing cardiovascular disease (i.due east. for chief prevention).[63] Statins decrease cholesterol in children with hypercholesterolemia, merely no studies every bit of 2010 show improved outcomes[65] and nutrition is the mainstay of therapy in childhood.[33]
Other agents that may exist used include fibrates, nicotinic acid, and cholestyramine.[66] These, however, are only recommended if statins are non tolerated or in pregnant women.[66] Injectable antibodies confronting the protein PCSK9 (evolocumab, bococizumab, alirocumab) can reduce LDL cholesterol and have been shown to reduce bloodshed.[67]
Guidelines [edit]
In the USA, guidelines exist from the National Cholesterol Education Plan (2004)[68] and a joint torso of professional societies led by the American Heart Association.[69]
In the UK, the National Constitute for Health and Clinical Excellence has made recommendations for the handling of elevated cholesterol levels, published in 2008,[66] and a new guideline appeared in 2014 that covers the prevention of cardiovascular disease in full general.[seventy]
The Task Force for the management of dyslipidaemias of the European Club of Cardiology and the European Atherosclerosis Society published guidelines for the management of dyslipidaemias in 2011.[33]
Specific populations [edit]
Among people whose life expectancy is relatively short, hypercholesterolemia is not a risk factor for death past any cause including coronary eye illness.[71] Among people older than 70, hypercholesterolemia is non a hazard gene for being hospitalized with myocardial infarction or angina.[71] There are also increased risks in people older than 85 in the apply of statin drugs.[71] Considering of this, medications which lower lipid levels should non be routinely used amongst people with express life expectancy.[71]
The American College of Physicians recommends for hypercholesterolemia in people with diabetes:[72]
- Lipid-lowering therapy should exist used for secondary prevention of cardiovascular mortality and morbidity for all adults with known coronary artery illness and type two diabetes.
- Statins should be used for primary prevention against macrovascular complications in adults with type 2 diabetes and other cardiovascular risk factors.
- Once lipid-lowering therapy is initiated, people with type 2 diabetes mellitus should be taking at to the lowest degree moderate doses of a statin.[73]
- For those people with type ii diabetes who are taking statins, routine monitoring of liver function tests or muscle enzymes is non recommended except in specific circumstances.
Alternative medicine [edit]
Co-ordinate to a survey in 2002, alternative medicine was used in an attempt to treat cholesterol by ane.1% of U.S. adults. Consistent with previous surveys, this one found the majority of individuals (55%) used it in conjunction with conventional medicine.[74] A systematic review[75] of the effectiveness of herbal medicines utilized in traditional chinese medicine had inconclusive results due to the poor methodological quality of the included studies. A review of trials of phytosterols and/or phytostanols, boilerplate dose ii.15 g/day, reported an boilerplate of 9% lowering of LDL-cholesterol.[76] In 2000, the Food and Drug Administration approved the labeling of foods containing specified amounts of phytosterol esters or phytostanol esters equally cholesterol-lowering; in 2003, an FDA Interim Wellness Claim Dominion extended that label merits to foods or dietary supplements delivering more than than 0.eight g/24-hour interval of phytosterols or phytostanols. Some researchers, all the same, are concerned well-nigh nutrition supplementation with establish sterol esters and draw attention to lack of long-term prophylactic data.[77]
Epidemiology [edit]
Rates of high total cholesterol in the Us in 2010 are but over 13%, down from 17% in 2000.[78]
Boilerplate total cholesterol in the Great britain is v.nine mmol/L, while in rural China and Nippon, average total cholesterol is 4 mmol/L.[10] Rates of coronary artery disease are high in United kingdom of great britain and northern ireland, simply low in rural China and Japan.[10]
Research directions [edit]
Gene therapy is beingness studied as a potential treatment.[79] [80]
References [edit]
- ^ a b c d Durrington, P (August 2003). "Dyslipidaemia". The Lancet. 362 (9385): 717–31. doi:ten.1016/S0140-6736(03)14234-i. PMID 12957096. S2CID 208792416.
- ^ Behrman, E. J.; Gopalan, Venkat (2005-12-01). "Cholesterol and Plants". Journal of Chemical Teaching. 82 (12): 1791. Bibcode:2005JChEd..82.1791B. doi:10.1021/ed082p1791. ISSN 0021-9584.
- ^ Biggerstaff KD, Wooten JS (December 2004). "Understanding lipoproteins as transporters of cholesterol and other lipids". Adv Physiol Educ. 28 (1–four): 105–06. doi:10.1152/advan.00048.2003. PMID 15319192.
- ^ Carmena R, Duriez P, Fruchart JC (June 2004). "Atherogenic lipoprotein particles in atherosclerosis". Circulation. 109 (23 Suppl 1): III2–seven. doi:x.1161/01.CIR.0000131511.50734.44. PMID 15198959.
- ^ Kontush A, Chapman MJ (March 2006). "Antiatherogenic small, dense HDL – guardian angel of the arterial wall?". Nat Clin Pract Cardiovasc Med. 3 (three): 144–53. doi:10.1038/ncpcardio0500. PMID 16505860. S2CID 27738163.
- ^ "Healthy diet – Fact canvas N°394". World Health Organisation. September 2015. Retrieved July 6, 2016.
- ^ a b c de Souza, RJ; Mente, A; Maroleanu, A; Cozma, AI; Ha, V; Kishibe, T; Uleryk, E; Budylowski, P; Schünemann, H; Beyene, J; Anand, SS (11 Baronial 2015). "Intake of saturated and trans unsaturated fatty acids and risk of all cause mortality, cardiovascular illness, and blazon 2 diabetes: systematic review and meta-analysis of observational studies". BMJ (Clinical Research Ed.). 351: h3978. doi:x.1136/bmj.h3978. PMC4532752. PMID 26268692.
- ^ a b c d e f Ito MK, McGowan MP, Moriarty PM (June 2011). "Management of familial hypercholesterolemias in adult patients: recommendations from the National Lipid Association Skillful Console on Familial Hypercholesterolemia". J Clin Lipidol. 5 (3 Suppl): S38–45. doi:10.1016/j.jacl.2011.04.001. PMID 21600528.
- ^ "Hypercholesterolemia". Genetics Home Reference . Retrieved 16 May 2016.
- ^ a b c d e f one thousand h i Bhatnagar D, Soran H, Durrington PN (2008). "Hypercholesterolaemia and its direction". BMJ. 337: a993. doi:x.1136/bmj.a993. PMID 18719012. S2CID 5339837.
- ^ Finn AV, Nakano M, Narula J, Kolodgie FD, Virmani R (July 2010). "Concept of vulnerable/unstable plaque". Arterioscler. Thromb. Vasc. Biol. 30 (7): 1282–92. doi:ten.1161/ATVBAHA.108.179739. PMID 20554950.
- ^ Grundy, SM; Balady, GJ; Criqui, MH; Fletcher, One thousand; Greenland, P; Hiratzka, LF; Houston-Miller, North; Kris-Etherton, P; Krumholz, HM; Larosa, J.; Ockene, I. S.; Pearson, T. A.; Reed, J.; Washington, R.; Smith, S. C. (1998). "Master prevention of coronary heart illness: guidance from Framingham: a statement for healthcare professionals from the AHA Task Force on Hazard Reduction. American Eye Association". Circulation. 97 (eighteen): 1876–87. doi:10.1161/01.CIR.97.18.1876. PMID 9603549.
- ^ Shields, C; Shields, J (2008). Eyelid, conjunctival, and orbital tumors: atlas and textbook. Hagerstown, Maryland: Lippincott Williams & Wilkins. ISBN978-0-7817-7578-vi.
- ^ Zech LA Jr; Hoeg JM (2008-03-10). "Correlating corneal arcus with atherosclerosis in familial hypercholesterolemia". Lipids Wellness Dis. seven (1): 7. doi:10.1186/1476-511X-7-7. PMC2279133. PMID 18331643.
- ^ a b James, WD; Berger, TG (2006). Andrews' Diseases of the Skin: Clinical Dermatology. Saunders Elsevier. pp. 530–32. ISBN978-0-7216-2921-6.
- ^ Rapini, RP; Bolognia, JL; Jorizzo, JL (2007). Dermatology: 2-Book Set. St. Louis, Missouri: Mosby. pp. 1415–16. ISBN978-i-4160-2999-1.
- ^ Calderon, R.; Schneider, R. H.; Alexander, C. N.; Myers, H. F.; Nidich, S. I.; Haney, C. (1999). "Stress, stress reduction and hypercholesterolemia in African Americans: a review". Ethnicity & Affliction. 9: 451–462. ISSN 1049-510X.
- ^ Cacioppo, J.; Hawkley, 50. (2010). "Loneliness Matters: A Theorectical and Empirical Review of Consequences and Mechanisms". Register of Behavioral Medicine. 40 (2): 218–227. doi:x.1007/s12160-010-9210-8. PMC3874845. PMID 20652462.
- ^ a b Mannu, GS; Zaman, MJ; Gupta, A; Rehman, HU; Myint, PK (ane February 2013). "Evidence of lifestyle modification in the management of hypercholesterolemia". Current Cardiology Reviews. 9 (i): two–14. doi:10.2174/157340313805076313. PMC3584303. PMID 22998604.
- ^ Howell WH, McNamara DJ, Tosca MA, Smith BT, Gaines JA (June 1997). "Plasma lipid and lipoprotein responses to dietary fat and cholesterol: a meta-analysis". Am. J. Clin. Nutr. 65 (6): 1747–64. doi:x.1093/ajcn/65.half dozen.1747. PMID 9174470.
- ^ DiNicolantonio, James J.; Lucan, Sean C.; O'Keefe, James H. (2016). "The Show for Saturated Fat and for Saccharide Related to Coronary Middle Disease". Progress in Cardiovascular Diseases. 58 (five): 464–472. doi:ten.1016/j.pcad.2015.11.006. ISSN 0033-0620. PMC4856550. PMID 26586275.
- ^ Ascherio A, Willett WC (October 1997). "Health effects of trans fatty acids". Am. J. Clin. Nutr. 66 (4 Suppl): 1006S–10S. doi:10.1093/ajcn/66.4.1006S. PMID 9322581.
- ^ Grundy, SM (November 2016). "Does Dietary Cholesterol Matter?". Electric current Atherosclerosis Reports. 18 (11): 68. doi:10.1007/s11883-016-0615-0. PMID 27739004. S2CID 30969287.
- ^ Vincent, Melissa J.; Allen, Bruce; Palacios, Orsolya Chiliad.; Haber, Lynne T.; Maki, Kevin C. (2019-01-01). "Meta-regression analysis of the effects of dietary cholesterol intake on LDL and HDL cholesterol". The American Journal of Clinical Diet. 109 (1): 7–xvi. doi:10.1093/ajcn/nqy273. ISSN 0002-9165. PMID 30596814.
- ^ Herink, Megan; Ito, Matthew K. (2000-01-01). "Medication Induced Changes in Lipid and Lipoproteins". In De Groot, Leslie J.; Chrousos, George; Dungan, Kathleen; Feingold, Kenneth R.; Grossman, Ashley; Hershman, Jerome M.; Koch, Christian; Korbonits, Márta; McLachlan, Robert (eds.). Endotext. Southward Dartmouth (MA): MDText.com, Inc. PMID 26561699.
- ^ "Hypercholesterolemia". Genetics Home Reference. U.S. National Institutes of Health. Retrieved 5 December 2013.
- ^ Akioyamen LE, Genest J, Shan SD, Reel RL, Albaum JM, Chu A; et al. (2017). "Estimating the prevalence of heterozygous familial hypercholesterolaemia: a systematic review and meta-analysis". BMJ Open up. 7 (9): e016461. doi:10.1136/bmjopen-2017-016461. PMC5588988. PMID 28864697.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b c d east f g h i j k Consumer Reports; Drug Effectiveness Review Project (March 2013). "Evaluating statin drugs to treat High Cholesterol and Centre Disease: Comparison Effectiveness, Safety, and Price" (PDF). Best Purchase Drugs. Consumer Reports: 9. Retrieved 27 March 2013. which cites
- United States Department of Health and Human Services; National Centre Lung and Blood Institute; National Institutes of Health (June 2005). "NHLBI, High Blood Cholesterol: What You Need to Know". nhlbi.nih.gov. Archived from the original on 1 Apr 2013. Retrieved 27 March 2013.
- ^ Loftier Cholesterol – Tests and Diagnosis, Mayo Clinic staff. Retrieved 2013-03-09.
- ^ Diagnosing High Cholesterol, NHS Choices. Retrieved 2013-03-09.
- ^ ATP III Guidelines At-A-Glance Quick Desk Reference, National Cholesterol Educational activity Program. Retrieved 2013-03-09.
- ^
- ^ a b c d eastward f g h Reiner Z, Catapano AL, De Backer G, et al. (July 2011). "ESC/EAS Guidelines for the management of dyslipidaemias: the Job Forcefulness for the management of dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Guild (EAS)". Eur. Heart J. 32 (xiv): 1769–818. doi:ten.1093/eurheartj/ehr158. PMID 21712404.
- ^ Friedewald WT, Levy RI, Fredrickson DS (June 1972). "Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without apply of the preparative ultracentrifuge". Clin Chem. eighteen (6): 499–502. PMID 4337382.
- ^ Youngblom, Emily; Pariani, Mitchel; Knowles, Joshua W. (1993), Adam, Margaret P.; Ardinger, Holly H.; Pagon, Roberta A.; Wallace, Stephanie E. (eds.), "Familial Hypercholesterolemia", GeneReviews®, Seattle (WA): Academy of Washington, Seattle, PMID 24404629, retrieved 2021-01-04
- ^ U.South. Preventive Services Chore Strength. "Screening for Lipid Disorders: Recommendations and Rationale". Archived from the original on 2015-02-10. Retrieved 2010-11-04 .
- ^ Chou Roger (9 August 2016). "Screening for Dyslipidemia in Younger Adults: A Systematic Review for the U.Due south. Preventive Services Task Force". Register of Internal Medicine. 165 (8): 560–564. doi:10.7326/M16-0946. PMID 27538032. S2CID 20592431.
- ^ Bibbins-Domingo, Kirsten; Grossman, David C.; Curry, Susan J.; Davidson, Karina W.; Epling, John W.; García, Francisco A. R.; Gillman, Matthew W.; Kemper, Alex R.; Krist, Alex H.; Kurth, Ann E.; Landefeld, C. Seth; Lefevre, Michael; Mangione, Ballad M.; Owens, Douglas K.; Phillips, William R.; Phipps, Maureen K.; Pignone, Michael P.; Siu, Albert 50. (August 9, 2016). "Screening for Lipid Disorders in Children and Adolescents". JAMA. 316 (half dozen): 625–33. doi:x.1001/jama.2016.9852. PMID 27532917.
- ^ Genest, J; Frohlich, J; Fodor, Chiliad; McPherson, R (2003-ten-28). "Recommendations for the direction of dyslipidemia and the prevention of cardiovascular affliction: summary of the 2003 update". Canadian Medical Association Periodical. 169 (ix): 921–iv. PMC219626. PMID 14581310.
- ^ National Cholesterol Education Plan (NCEP), Iii) (2002-12-17). "Third Study of the National Cholesterol Education Program (NCEP) Practiced Panel on Detection, Evaluation, and Treatment of Loftier Claret Cholesterol in Adults (Adult Treatment Panel III) concluding written report". Circulation. 106 (25): 3143–421. doi:x.1161/circ.106.25.3143. hdl:2027/uc1.c095473168. PMID 12485966.
- ^ Spector, R; Snapinn, SM (2011). "Statins for secondary prevention of cardiovascular disease: the right dose". Pharmacology. 87 (1–ii): 63–69. doi:x.1159/000322999. PMID 21228612.
- ^ a b c d Grundy, SM; Cleeman, JI; Merz, CN; Brewer HB, Jr; Clark, LT; Hunninghake, DB; Pasternak, RC; Smith SC, Jr; Rock, NJ (Jul 13, 2004). "Implications of contempo clinical trials for the National Cholesterol Education Program Adult Treatment Panel 3 guidelines". Circulation. 110 (two): 227–39. doi:ten.1161/01.cir.0000133317.49796.0e. PMID 15249516.
- ^ Consumer Reports; Drug Effectiveness Review Project (March 2013). "Evaluating statin drugs to treat High Cholesterol and Heart Disease: Comparison Effectiveness, Condom, and Cost" (PDF). Best Buy Drugs. Consumer Reports: 9. Retrieved 27 March 2013.
- ^ Bhattarai, N; Prevost, AT; Wright, AJ; Charlton, J; Rudisill, C; Gulliford, MC (20 December 2013). "Effectiveness of interventions to promote salubrious diet in primary intendance: systematic review and meta-analysis of randomised controlled trials". BMC Public Health. thirteen: 1203. doi:ten.1186/1471-2458-13-1203. PMC3890643. PMID 24355095.
- ^ Hartley, L; Igbinedion, Eastward; Holmes, J; Flowers, N; Thorogood, Chiliad; Clarke, A; Stranges, S; Hooper, L; Rees, Chiliad (4 June 2013). "Increased consumption of fruit and vegetables for the chief prevention of cardiovascular diseases". The Cochrane Database of Systematic Reviews. 2021 (6): CD009874. doi:10.1002/14651858.CD009874.pub2. PMC4176664. PMID 23736950.
- ^ a b Brownawell, Amy 1000.; Falk, Michael C. (2010-06-01). "Cholesterol: where scientific discipline and public health policy intersect". Nutrition Reviews. 68 (6): 355–64. doi:10.1111/j.1753-4887.2010.00294.10. ISSN 1753-4887. PMID 20536780.
- ^ Berger, Samantha; Raman, Gowri; Vishwanathan, Rohini; Jacques, Paul F.; Johnson, Elizabeth J. (2015-08-01). "Dietary cholesterol and cardiovascular disease: a systematic review and meta-analysis". The American Journal of Clinical Nutrition. 102 (2): 276–94. doi:10.3945/ajcn.114.100305. ISSN 1938-3207. PMID 26109578.
- ^ Keys, Ancel; Anderson, Joseph T; Grande, Francisco (July 1965). "Serum cholesterol response to changes in the nutrition: 4. Particular saturated fatty acids in the nutrition". Metabolism. fourteen (7): 776–87. doi:10.1016/0026-0495(65)90004-ane. ISSN 0026-0495. PMID 25286466.
- ^ Hegsted, DM; McGandy, RB; Myers, ML; Stare, FJ (November 1965). "Quantitative effects of dietary fat on serum cholesterol in human". The American Periodical of Clinical Nutrition. 17 (v): 281–95. doi:ten.1093/ajcn/17.5.281. ISSN 0002-9165. PMID 5846902.
- ^ The 2015 Dietary Guidelines Informational Committee (2015). "Scientific Report of the 2015 Dietary Guidelines Informational Committee" (PDF). wellness.gov. p. 17. Retrieved sixteen May 2016.
The 2015 DGAC will not bring frontward this recommendation 644 because available evidence shows no appreciable relationship between consumption of dietary cholesterol and serum cholesterol, consistent with the conclusions of the AHA/ACC study.
- ^ Hooper, Lee; Martin, Nicole; Jimoh, Oluseyi F.; Kirk, Christian; Foster, Eve; Abdelhamid, Asmaa South. (21 August 2020). "Reduction in saturated fat intake for cardiovascular disease". The Cochrane Database of Systematic Reviews. eight: CD011737. doi:x.1002/14651858.CD011737.pub3. ISSN 1469-493X. PMC8092457. PMID 32827219.
- ^ Chowdhury, R; Warnakula, S; Kunutsor, S; Crowe, F; Ward, HA; Johnson, Fifty; Franco, OH; Butterworth, AS; Forouhi, NG; Thompson, SG; Khaw, KT; Mozaffarian, D; Danesh, J; Di Angelantonio, E (18 March 2014). "Association of dietary, circulating, and supplement fat acids with coronary risk: a systematic review and meta-analysis". Annals of Internal Medicine. 160 (6): 398–406. doi:x.7326/M13-1788. PMID 24723079.
- ^ Schwingshackl, Fifty; Hoffmann, G (December 2013). "Comparison of effects of long-term low-fatty vs high-fat diets on blood lipid levels in overweight or obese patients: a systematic review and meta-assay". Periodical of the University of Nutrition and Dietetics. 113 (12): 1640–61. doi:ten.1016/j.jand.2013.07.010. PMID 24139973.
Including only hypocaloric diets, the effects of low-fat vs high-fat diets on total cholesterol and LDL cholesterol levels were abolished.
- ^ Brown, Lisa; Rosner, Bernard; Willett, Walter W.; Sacks, Frank M. (1999-01-01). "Cholesterol-lowering effects of dietary fiber: a meta-analysis". The American Journal of Clinical Nutrition. 69 (i): thirty–42. doi:ten.1093/ajcn/69.1.30. ISSN 0002-9165. PMID 9925120.
- ^ Hollænder, Pernille LB; Ross, Alastair B.; Kristensen, Mette (2015-09-01). "Whole-grain and blood lipid changes in plainly healthy adults: a systematic review and meta-assay of randomized controlled studies". The American Journal of Clinical Nutrition. 102 (iii): 556–72. doi:10.3945/ajcn.115.109165. ISSN 0002-9165. PMID 26269373.
- ^ Schaefer, EJ; Gleason, JA; Dansinger, ML (June 2009). "Dietary fructose and glucose differentially affect lipid and glucose homeostasis". The Journal of Diet. 139 (half-dozen): 1257S–62S. doi:10.3945/jn.108.098186. PMC2682989. PMID 19403705.
- ^ Grundy, Scott Yard.; Stone, Neil J.; Bailey, Alison L.; Beam, Craig; Birtcher, Kim M.; Blumenthal, Roger S.; Braun, Lynne T.; de Ferranti, Sarah; Faiella-Tommasino, Joseph (2018-eleven-x). "2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Blood Cholesterol: A Study of the American Higher of Cardiology/American Heart Association Task Strength on Clinical Exercise Guidelines". Circulation. 139 (25): e1082–e1143. doi:x.1161/CIR.0000000000000625. ISSN 0009-7322. PMC7403606. PMID 30586774.
- ^ Windecker, Stephan; Mach, François; Räber, Lorenz; Mavridis, Dimitris; Piccolo, Raffaele; Siontis, George C. M.; Koskinas, Konstantinos C. (2018-04-07). "Effect of statins and non-statin LDL-lowering medications on cardiovascular outcomes in secondary prevention: a meta-analysis of randomized trials". European Centre Journal. 39 (fourteen): 1172–1180. doi:ten.1093/eurheartj/ehx566. ISSN 0195-668X. PMID 29069377.
- ^ Tonelli, M; Lloyd, A; Cloudless, F; Conly, J; Husereau, D; Hemmelgarn, B; Klarenbach, South; McAlister, FA; Wiebe, Due north; Manns, B (2011-11-08). "Efficacy of statins for primary prevention in people at low cardiovascular risk: a meta-analysis". CMAJ : Canadian Medical Association Journal. 183 (16): E1189–E1202. doi:10.1503/cmaj.101280. PMC3216447. PMID 21989464.
- ^ Mills, EJ; Wu, P; Chong, G; Ghement, I; Singh, S; Akl, EA; Eyawo, O; Guyatt, G; Berwanger, O; Briel, K (February 2011). "Efficacy and safety of statin treatment for cardiovascular disease: a network meta-assay of 170,255 patients from 76 randomized trials". QJM: Monthly Journal of the Association of Physicians. 104 (2): 109–24. doi:10.1093/qjmed/hcq165. PMID 20934984.
- ^ Cholesterol Treatment Trialists' (CTT) Collaborators (2012). "The effects of lowering LDL cholesterol with statin therapy in people at depression chance of vascular disease: meta-analysis of individual data from 27 randomised trials". Lancet. 380 (9841): 581–90. doi:10.1016/S0140-6736(12)60367-5. PMC3437972. PMID 22607822.
- ^ Jeanne, Thomas L.; Daeges, Monica; Blazina, Ian; Dana, Tracy; Chou, Roger (2016-11-15). "Statins for Prevention of Cardiovascular Affliction in Adults: Show Study and Systematic Review for the U.s. Preventive Services Task Force". JAMA. 316 (19): 2008–2024. doi:ten.1001/jama.2015.15629. ISSN 0098-7484. PMID 27838722.
- ^ a b Taylor, Fiona; Huffman, Marking D; Macedo, Ana Filipa; Moore, Theresa HM; Burke, Margaret; Davey Smith, George; Ward, Kirsten; Ebrahim, Shah (2013-01-31). "Statins for the primary prevention of cardiovascular disease". Cochrane Database of Systematic Reviews. 2021 (1): CD004816. doi:10.1002/14651858.cd004816.pub5. ISSN 1465-1858. PMC6481400. PMID 23440795.
- ^ Adept Opin Pharmacother. 2015 Feb;sixteen(3):347–56. doi: x.1517/14656566.2014.986094. Epub 2014 Dec 5. Ongoing challenges for pharmacotherapy for dyslipidemia. Pisaniello Advertizement, Scherer DJ, Kataoka Y, Nicholls SJ.
- ^ Lebenthal Y, Horvath A, Dziechciarz P, Szajewska H, Shamir R (2010). "Are treatment targets for hypercholesterolemia evidence based? Systematic review and meta-analysis of randomised controlled trials". Curvation Dis Child. 95 (ix): 673–fourscore. doi:10.1136/adc.2008.157024. PMID 20515970. S2CID 24263653.
- ^ a b c National Institute for Health and Clinical Excellence. Clinical guideline 67: Lipid modification. London, 2008.
- ^ Grundy SM, Cleeman JI, Merz CN, Brewer HB, Clark LT, Hunninghake DB, Pasternak RC, Smith SC, Rock NJ (2004). "Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel Iii Guidelines". J Am Coll Cardiol. 44 (three): 720–32. doi:ten.1016/j.jacc.2004.07.001. PMID 15358046.
- ^ Grundy, SM; Stone, NJ; Bailey, AL; Beam, C; Birtcher, KK; Blumenthal, RS; Braun, LT; de Ferranti, S; Faiella-Tommasino, J; Forman, DE; Goldberg, R; Heidenreich, PA; Hlatky, MA; Jones, DW; Lloyd-Jones, D; Lopez-Pajares, Due north; Ndumele, CE; Orringer, CE; Peralta, CA; Saseen, JJ; Smith SC, Jr; Sperling, L; Virani, SS; Yeboah, J (x Nov 2018). "2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Blood Cholesterol: Executive Summary". Circulation. 139 (25): e1046–e1081. doi:10.1161/CIR.0000000000000624. PMID 30565953.
- ^ National Institute for Wellness and Clinical Excellence. "Cardiovascular disease: risk assessment and reduction, including lipid modification". Nice . Retrieved 27 May 2019.
- ^ a b c d AMDA – The Gild for Post-Astute and Long-Term Care Medicine (February 2014), "Ten Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, AMDA – The Social club for Mail service-Acute and Long-Term Intendance Medicine, retrieved 20 April 2015
- ^ Snow 5, Aronson M, Hornbake E, Mottur-Pilson C, Weiss K (2004). "Lipid control in the direction of type 2 diabetes mellitus: a clinical practice guideline from the American College of Physicians". Ann Intern Med. 140 (8): 644–49. doi:10.7326/0003-4819-140-8-200404200-00012. PMID 15096336. S2CID 6744974.
- ^ Vijan, Due south; Hayward, RA; American College Of, Physicians (2004). "Pharmacologic lipid-lowering therapy in blazon 2 diabetes mellitus: background paper for the American College of Physicians". Ann Intern Med. 140 (8): 650–58. doi:10.7326/0003-4819-140-8-200404200-00013. PMID 15096337.
- ^ Barnes PM, Powell-Griner E, McFann G, Nahin RL (May 27, 2004). "Complementary and Culling Medicine Use Amongst Adults: United States, 2002" (PDF). Advance Data from Vital and Health Statistics. http://nccih.nih.gov/news/2004/052704.htm (343): 6–9. Retrieved 2010-11-04 .
- ^ Liu, Zhao Lan; Liu, Jian Ping; Zhang, Anthony Lin; Wu, Qiong; Ruan, Yao; Lewith, George; Visconte, Denise (2011-07-05). Cochrane Metabolic and Endocrine Disorders Grouping (ed.). "Chinese herbal medicines for hypercholesterolemia". Cochrane Database of Systematic Reviews (7): CD008305. doi:10.1002/14651858.CD008305.pub2. PMC3402023. PMID 21735427.
- ^ Demonty I, Ras RT, van der Knaap HC, Duchateau GS, Meijer L, Zock PL, Geleijnse JM, Trautwein EA (February 2009). "Continuous dose-response human relationship of the LDL-cholesterol-lowering consequence of phytosterol intake". J Nutr. 139 (2): 271–84. doi:10.3945/jn.108.095125. PMID 19091798.
- ^ Weingärtner O.; Bohm, Thousand.; Laufs, U.; et al. (2009). "Controversial part of plant sterol esters in the management of hypercholesterolaemia". European Heart Journal. 30 (4): 404–09. doi:ten.1093/eurheartj/ehn580. PMC2642922. PMID 19158117.
- ^ Carrol, Margaret (Apr 2012). "Full and High-density Lipoprotein Cholesterol in Adults: National Health and Nutrition Test Survey, 2009–2010" (PDF). CDC.
- ^ Van Craeyveld E, Jacobs F, Gordts SC, De Geest B (2011). "Cistron therapy for familial hypercholesterolemia". Curr Pharm Des. 17 (24): 2575–91. doi:x.2174/138161211797247550. PMID 21774774.
- ^ Al-Allaf FA, Coutelle C, Waddington SN, David AL, Harbottle R, Themis M (2010). "LDLR-Factor therapy for familial hypercholesterolaemia: problems, progress, and perspectives". Int Arch Med. three: 36. doi:10.1186/1755-7682-3-36. PMC3016243. PMID 21144047.
External links [edit]
Source: https://en.wikipedia.org/wiki/Hypercholesterolemia

0 Response to "Power Transformation on Powertransform(Cbind(Chol,hdl,ratio,glyhb,height)~1, Family="Yjpower",diab)"
Post a Comment